Accidental digitoxin intoxication: an interplay between laboratory and clinical medicine
Luigi M. Castello
[1]
Sophie Negro
[1]
Francesca Santi
[1]
Isabella Zanotti
[1]
Matteo Vidali
[*]
[2]
Marco Bagnati
[2]
Giorgio Bellomo
[2]
Gian Carlo Avanzi
[1]
Introduction
Cardiac glycoside poisoning is a potentially life-threatening problem which frequently occurs in patients on digitalis or following deliberate or fortuitous ingestion of leaves of Digitalis lanata (Woolly foxglove), Digitalis purpurea (Common foxglove), or other plants, containing molecules with similar effects, collected from home-grown gardens for homemade herbal preparations (1-3). In some reported cases glycoside ingestion was due to erroneous identification of leaves, not always easily distinguishable from those of other edible plants (3). Whereas a typical clinical presentation of digitalis toxicity in a patient on digitalis may easily address a relatively simple diagnosis, difficulties arise in case of unintentional poisoning. Laboratory tests based on anti-digoxin antibodies are widely available and significantly support the clinician in establishing the diagnosis; however these immunoassays frequently rely on monoclonal antibodies which do not cross-react to other cardioactive glycosides, potentially delaying or complicating diagnosis and therapy (4,5). Further complexity is due to heterogeneity of glycosides present in different plants, either as percentage amount or as chemical properties and pharmacokinetics (1,3).
Aim of this work is to show the importance that the clinical approach still has in the emergency setting and to emphasize how the interplay between laboratory and clinicians may guide or support patient treatment.
Case report
A married couple (a 61 year old man and his wife aged 60) arrived at the Maggiore della Carità Hospital (Novara, Italy) because of diarrhea, nausea and vomiting for 4 days; they also complained weakness, fatigue and visual hallucinations (orange and purple halo around lights). The subjects reported the ingestion of some leaves of a plant that they supposed to be "donkey ears" (Plantago minor; scientific name Plantago lanceolata) a week before; they collected these herbs still in leaf buds and used them for tea and for a pasta sauce.
In the emergency room physical examination showed bradycardia in both, most pronounced in the male (35/min) combined with hypotension (80/60 mmHg blood pressure). ECG examination disclosed sinus rhythm and repolarization abnormalities (scooping of the ST-T complex) in both and a 2:1 AV block was detected in the male patient. He was treated with atropine (two doses of 0.5 mg, i. v.) without any effect.
ECG pattern, history and clinical findings were consistent with digitalis toxicity (6), but standard plasma digoxin assay was repeatedly negative for both patients (both at the admission and after 4 hours). Nonetheless, given the high probability of digitalis toxicity, even if not confirmed by a laboratory test, after consulting with the clinical pathologist that could not exclude or confirm at that time glycoside intoxication, the male patient was treated with anti-digoxin antibodies (Digifab®, Digoxin Immune Fab (Ovine), 3 vials containing 40 mg of antibody each, infused i. v. in 30 minutes), in addition to supportive care (6-10). The AV block was reverted in two hours after the beginning of treatment. Anti-digoxin antibodies were not administered to woman because she was clinically stable.
The presence of cardiac glycosides in plasma of both patients was subsequently confirmed by Liquid Chromatography-Mass Spectrometry (LC-MS/MS) (11,12). Digitoxin was identified in both patients (woman: 50 ng/mL, man: 100 ng/mL) at toxic plasma levels compatible with the severity of the clinical picture (digitoxin therapeutic range: 10-30 ng/mL) (Figure 1). Colchicines and protoveratine, as possible alternative toxic drugs, were excluded by LC-MS/MS patient plasma analysis. Digoxin was confirmed as negative by LC-MS/MS. After 48 hours of monitoring, both patients were discharged. Interestingly, a sample of the plants collected by the couple, brought to the Hospital some weeks later, was analyzed by an expert botanist and found to be Digitalis purpurea.
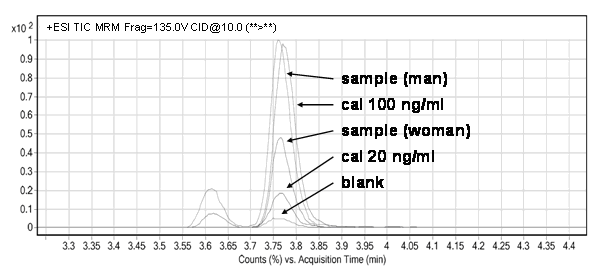
Figure 1. LC-MS/MS digitoxin chromatographic assay.
At 3.77 min, from bottom to top, it is possible to observe chromatographic peaks corresponding respectively to blank, digitoxin standard sample at 20 ng/mL, female sample (50 ng/mL), digitoxin standard sample at 100 ng/mL and male sample (100 ng/mL).
Materials and methods
Digoxin testing
Digoxin test was performed by the automated immunoassay system ADVIA Centaur® by Siemens Healthcare Diagnostics Inc (Deerfield, IL, USA). ADVIA Centaur Digoxin test is a commercial competitive immunoassay using direct chemiluminescent technology. Digoxin in the patient sample competes for a limited amount of acridinium ester-labeled monoclonal mouse anti-digoxin antibody. Cross-reactivity to digitoxin, precision and limit of detection, as declared by the Manufactures, are respectively < 1%, 3-5.5% and 0.1ng/mL. Digoxin concentration was evaluated twice for each patient (at the admission and after 4 hours) using BD Vacutainer® Lithium Heparin tubes.
Digitoxin test by LC/MS/MS
Digitoxin (purity ≥ 92% (HPLC) powder) was purchased from Sigma-Aldrich (St. Louis, MO, USA). LiChrosolv® water (for LC-MS) and LiChrosolv® hypergrade acetonitrile (for LC/MS) were purchased from Merck (Darmstadt, Germany). All other solvents were of analytical grade or HPLC grade when appropriate. Sample preparation was slightly modified from the method of Xue et al. (12). Briefly, digitoxin was dissolved in methanol:water (50:50, v/v) and standard solutions or homemade controls were obtained by spiking blank plasma. 500 μL of plasma (blank, calibrators, controls or samples) and 100 μL of ammonium hydroxide were mixed with 5 mL of ter-butylmethylether. After centrifugation, 4 mL of supernatant were evaporated and mixed with 300 μL of water:acetonitrile (50:50). The LC-MS/MS system consisted of an Agilent 6410 triple-quadrupole mass spectrometer (Agilent Technologies Inc., Santa Clara, CA, USA) equipped with ESI interface and an HPLC Agilent 1290 Infinity (digitoxin transition: 782.5>635.5; fragmentor 135; collision energy 10). LC-MS/MS parameters were optimized by injecting a solution of digitoxin 1 mg/mL in methanol:water. Analytes were separated at 50 °C on a Zorbax Eclipse XDB-C18 column (2.1 mm x 50 mm; 1.8 µm) using elution gradient of 5 mM ammonium formate, 0.01% formic acid in water (buffer A) and formic acid 0.01% in acetonitrile (buffer B). A partial and rapid validation process was performed. Selectivity was tested by analysing blank plasma obtained from different sources and no significant interference was observed at the expected retention time. Method linearity was verified up to 200 ng/mL using replicates at different concentrations (different sample preparative). Precision ranged over 7-10% and recovery, following liquid–liquid extraction procedure, ranged over 80-85%.
Digifab® treatment
Digifab® (Digoxin Immune Fab (Ovine), Protherics Inc. Brentwood, TN USA) is a purified preparation of immunoglobulin fragments with high digoxin affinity, obtained from healthy sheep immunized with a digoxin analogue. The drug, designed specifically for digoxin poisoning, acts also in cases of digitoxin and other cardiac glycoside overdose. Digifab® works through a competitive mechanism since its affinity for digoxin is greater than the affinity of digoxin for the sodium-potassium pump receptor. Digifab®, cleared primarily by kidneys (plasma half-life of 15-20 hours), acts rapidly (1-2 hours) and is usually administered by slow intravenous infusion (2,4). In this case 3 vials, containing 40 mg of antibody each, were infused i. v. in 30 minutes.
Discussion
Two critical aspects should be mentioned here. Firstly, in the emergency setting, where urgent decisions are needed, careful history and complete physical examination are still the most important tools for proper diagnosis and should guide patient treatment, even when clinician is not supported by laboratory data or when more sophisticated tests are not readily available. Secondly, in these last years laboratory systems have rapidly evolved with the development of newer instruments and more sensitive and specific assays. LC-MS/MS is now available in many hospitals, routinely used for therapeutic drug monitoring, and may be easily applied to clinical toxicology, particularly to the targeted screening of several toxic compounds. Although this technology may not be available 24 hours a day, it can support clinician’s decision even when medical treatment has already been initiated, as shown here. An undetectable plasma level of digoxin in the presence of typical ECG and clinical presentation may be confusing for the clinician, particularly when he could falsely assume that a digoxin test could also detect other cardiac glycosides. However, whereas polyclonal antibodies constituting Digifab® recognize a large spectrum of cardiac glycosides (it has been successfully used to treat life-threatening digitoxin overdose), digoxin determination frequently is based on monoclonal antibodies which do not cross-react to digitoxin. Due to the rapid development of new diagnostic tests, it can be difficult for the clinician to know the method by which analytical data have been obtained, as well as drawbacks and limitations, and ultimately how to correctly translate laboratory data into sound clinical information. In such a complexity, it is highly recommended to always discuss unexpected results with the laboratory physician. A critical point is why digoxin was not identified by immunoassay and did not appear in LC-MS/MS even if Digitalis purpurea contains digitoxin as well as digoxin. A possible explanation may be found in the different half-life of these two substances (30-50 hours for digoxin vs. 5-8 days for digitoxin) (3,13). With this regard, plants were consumed some days before arriving at the emergency department and, since the standard laboratory test for digoxin gave negative results, the clinician decided to measure digitoxin in the hypothesis that, due to its longer half-life, this cardiac glycoside would have been still present and responsible for the clinical picture. Although anti-heterophile antibodies present in human plasma could theoretically interfere with digoxin ADVIA Centaur immunoassay, possibly leading to both a falsely high or a falsely low result, this was not the case here because undetectable digoxin levels were also confirmed by LC-MS/MS.
In conclusion, in addition to the primary role of the clinical approach to patients in the emergency setting, this case report emphasizes how an active communication and a continuous sharing of professional experiences between laboratory and clinicians may ensure an early and correct diagnosis and guide or support patient treatment.



