Introduction
At the beginning of the 21st century there are defined priorities in laboratory medicine such as laboratory automation, laboratory consolidation, molecular diagnostics, imaging analysis, POCT, economics and accreditation of laboratories aiming to improve the quality of patient care. Quality in the health care is the level of excellence of the health care provided in relation to the current level of knowledge and technical development with customer orientation.
The main indicators of health care quality are the health of the population, equal opportunities in access to health care, effective provision of services, the efficiency and accessibility of the system and also the results of the health care provided. Lifestyle, genetic and environmental factors have a much higher influence on the health of the population than health care itself.
Regulation through quality in the health care sector is based on accreditation, certification, quality monitoring, patients’ rights, standard operation processes and standards of health care quality.
Laboratory medicine is backbone in the medical treatment, diagnosis and prevention. Laboratory diagnostics influence 70–80% of hospital health care decisions and costs between 3–5% of total health care costs.
Laboratory attempts to improve quality aim to reduce diagnostic errors and decrease turn around time with traceability of all laboratory procedures and to assure the safety of patients and staff alike; they concentrate on “tailor-made” or personalised medicine, striving for the highest possible quality service. Basic requirements and criteria for laboratories from client’s perspective are availability, comprehensiveness, fast response, reliability and accuracy, information and consultation as well as analysis of complaints and claims.
First systems or level of quality management systems in labs are internal and external quality control and educational activities which are the core points in all accreditations systems in labs.
The concept of laboratory accreditation is defined by ISO/IEC as formal recognition that the testing laboratory is competent to carry out specific tests or specific types of tests. Test is defined as a technical operation that consists of determination of one or more characteristics of a given product, process, or service according to a specified procedure. This is not quite appropriate for clinical laboratory. An importance set of criteria was done in EN 45 001 (European Standard), specifying general criteria for the operation of a testing laboratory. The accreditation body must be legally identifiable, impartial, and independent of external influences (1).
Next standard for accreditation was documented in ISO 17025 (General Requirements for the Competence of Testing and Calibration Laboratories) (2). This standard is widely used for testing laboratories in whole world in industry and also in medicine. The ISO 17025:2005 is the basis for the accreditation. This standard not only requires a management system and manual in the laboratory but also requires that the laboratory be found competent to perform specific tests/calibrations or types of tests/calibration.
Concerning quality, the strategic plans of IFCC and EFCC include focusing of accreditation of labs based on ISO standards and cooperation with European Accreditation and national accreditation bodies. IFCC recognises that ISO 15189:2007 – Medical laboratories – Particular requirements for quality and competence (3), encompasses all the assessment criteria specified in the policy statement and as such should form the basis for the accreditation of laboratories.
Accreditation in the world
Accreditation is done in several countries by independent National Accreditation Bodies. The situation of Europe was presented at the First European symposium on Quality Management in Laboratory Medicine, held in Paris in February 2009.
United Kingdom: CPA/UKAS partnership developed in 1996 and CPA standards were incorporating ISO 15189 requirements and the future development of accreditation consider the use of ISO 15189.
USA: The main program is CLIA (Clinical Laboratory Improvement Amendment) certification, but this program is far for the rules of accreditation based on ISO 15189.
Netherlands: The first Guidance document about quality was published in 1991 and the experts set the specific Accreditation Body for Medical Laboratories – CCKL in 1994. This body became as a division (of health) of national accreditation body in the Netherlands in 2008. The process of accreditation is voluntary, but more then 90% of clinical chemistry labs are accredited.
Germany: Quality assessment of quantitative measurements in medical laboratories has been regulated by the directive of German Federal Medical Board since 1971. In the most recent edition of RiLiBAK a new chapter has been added that prescribes quality requirements on the basis ISO 15189. Three accreditation bodies will be joint together based on EU rules that one country has only one national accreditation body. Accreditation is still performed voluntarily and around 20% of labs are accredited (4).
Sweden: Quality system management was implemented from 1989 (ISO Guide 25, EN 45001, ISO 17025 and 15189). Accreditation is on voluntary basis but it is the key part for health care insurance companies for the contract and reimbursement of expenses for health care.
Belgium: Clinical laboratories must be licensed by Ministry of Health and quality manual was adopted in the royal decree in 1999. There is close cooperation between professional society and BELAC (National Accreditation Body). A mandatory quality system based on the requirements of ISO 15189 but no formal accreditation is required. Formal accreditation becomes more and more conditional for reimbursement of laboratory tests.
France: According the decision of Ministry of Health all clinical labs must be accredited (ISO 15189) by COFRAC (National Accreditation Body) to the end of 2010.
Finland: In early 1990s, a working group in lab quality published guidelines on how to create a duality manual for clinical laboratories. Clinical labs have been mainly accredited by national Accreditation Body (FINAS) under ISO 17025, but ISO 15189 is also used (5).
Italy: In fact, Italy is divided into 20 regions, each of them having a different quality requirements, even when they are within the frame of a national health service and a set so called „minimal requirements“. The requirements are based on criteria inspired by the ISO 9001 standard and some laboratories are certified according this standard. A small number of laboratories applied for a CPA UK accreditation. Now, the ISO 15189 is considered to be the reference standard for accreditation, but the accreditation body dedicated to clinical laboratories does not exit (6).
Korea: The Korean Laboratory Accreditation Program (KLAP) was started in 1999 and this program based on national algorithm using guidelines, checklist, inspections etc. (7).
Canada: Accreditation of medical laboratories in Canada is regulated by provincial health authorities, five of them having accreditation bodies. Each of the bodies has developed its own standards implementing ISO documents. Canadian Coalitionfor Quality in Laboratory Medicine (CCQLM) has recently been incorporated to provide a national structure for harmonisation across Canada (8).
Croatia: The process of improvement quality is organised by national society (Croatian Society of Medical Biochemists) and professional chamber (Croatian Chamber of Medical Biochemists) and also with cooperation with national accreditation body. Currently, three labs are accredited according to ISO 15189 standard (9).
Czech Republic: The first meeting focusing only on the system of clinical labs accreditation was in 2000. There was discussion which way of implementation of QMS would be effective – ISO or national standards. Now, the accreditation of clinical labs is provided by Czech Institute of Accreditation (ISO 15189 preferable), and Czech Medical Association established NASKL (National Authorization Centre for Clinical Labs) with the aim to prepare the labs for accreditation according to ISO 15189. During this educational process the NASKL issues the certificate – Audit I and Audit II. There is a voluntary system but accreditation becomes more and more conditional for reimbursement of laboratory tests for health care insurance companies.
Accreditation according ISO 15189:2007 – Medical laboratories – Particular requirements for quality and competence
Accreditation is a procedure by which an authoritative body gives formal recognition that a body or person is competent to carry out specific tasks, it is an independent process (10,11).
The inspiration for national standards are ISO documents (ISO 9001, ISO 17025, ISO 15189) all around the world. The gold standard is ISO 15189 for clinical laboratories accreditation in Europe.
Main parts of ISO 15189:2007 and short comments
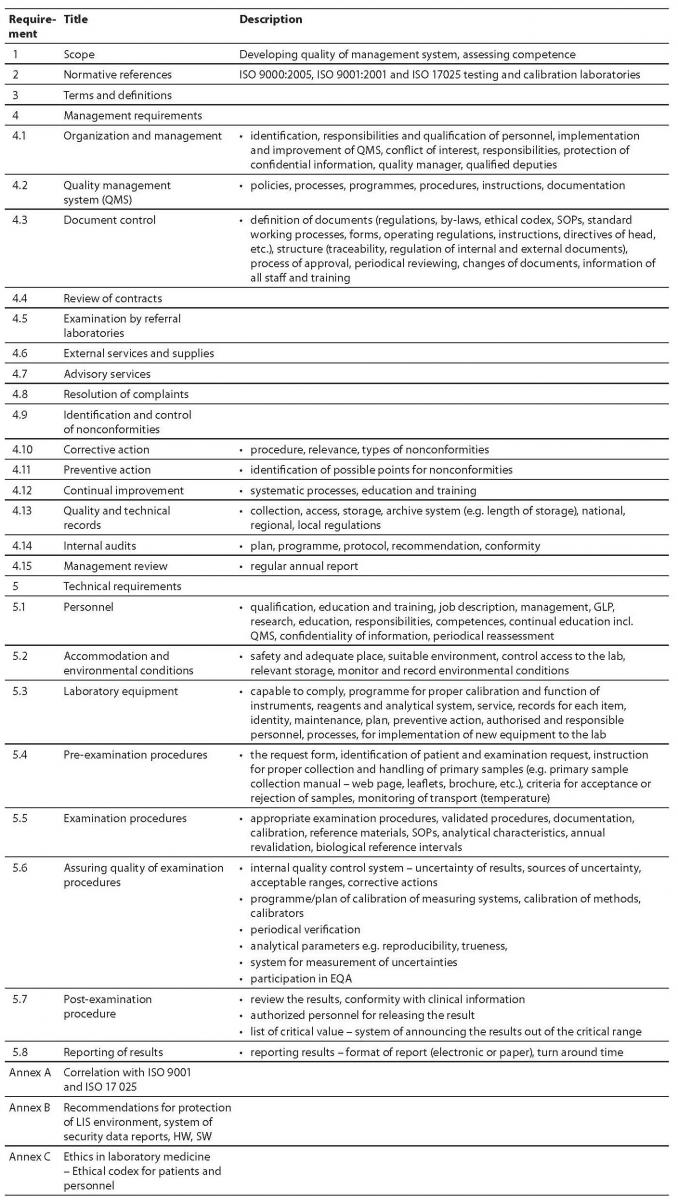
The main parts of ISO 15189:2007 and short comments are presented in table 1.
Table 1. Main parts of ISO 15189:2007 and short comments.
Accreditation process
To accredit or not to accredit, that is the question! The reason to start the process of accreditation would be interest in improvement of quality of lab services with better documentation of processes and responsibilities or interest of management(institute, hospital, owner, government, etc.), sometimes somebody should start after long time discussion about the quality.
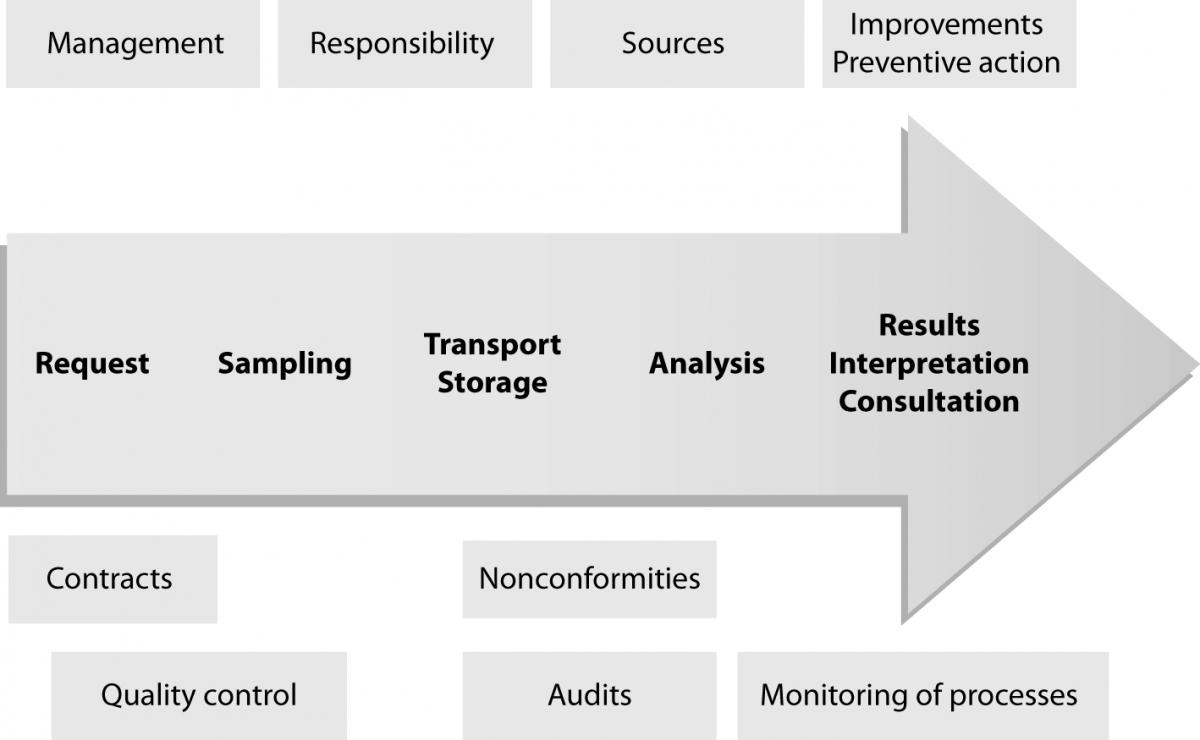
The first step before accreditation is building enthusiastic team with education on quality management system. Other steps include selection of methods, describing the processes in the lab, developing or improving the metrology system, definition and structure of documents, preparation of a quality manual, SOPs, etc. (Figure 1).
Figure 1. Map of accreditation process.
Somebody described the accreditation process: “Do the right things right, describe how you do it, do the things as you describe and evaluate everything.”
We should summarize that accreditation process has some benefits for labs as standardization of all processes, responsibility of each member of team, personal policy, demonstrability of results, systematic evaluation of suppliers, prestigious, better communication with partners (12). Never the process has only positive features, and also the negatives of accreditation exist, such as investments to education, to equipment and facilities, expenses on accreditation and consultation bodies and spent time of each member of staff. The accreditation improves the processes in the laboratories, increasing the quality in all areas in labs – reduction of errors in the pre-analytical processes, facilitation of accurate and rapid diagnosis, participation in acceleration and efficiency of treatment, facilitation of personalised medicine development, continuous improvement.
We need standardization of process of improving quality systems. The national systems should be suitable and tailored-made for national specifics and modalities (types of labs, etc.) but in global world we need one accreditation systems which now presents by ISO 15189 and all experts around the world know the expectations of system inside of laboratory.
Laboratory services will be the centre of attention regarding quality due to their wide ranging impact on patient care. Accreditation is not about who the best is, but who has a system of standard procedures. Accreditation is an instrument rather than aim, which increases the quality with high standard of services for clients – patients, physicians. Quality system is about people, with people and for people.
Acknowledgements
The study was supported by research project VZ MZO 000 64165 (MZ0VFN 2005).
Notes
Potential conflict of interest
None declared.
References
1. Dybkaer R. Quality Assurance, Accreditation, and Certification: Needs and Possibilities. Clin Chem 1994;40:1416-20.
2. EN ISO 17025:2005 General Requirements for the Competence of Testing and Calibration Laboratories.
3. EN ISO 15189:2007 – Medical laboratories – Particular requirements for quality and competence.
4. Kessler A. Laboratory quality regulations and accreditation standards in Germany. Clin Biochem 2009;42:315.
5. Laitinen P. Laboratory and quality regulations and accreditation standards in Finland. Clin Biochem 2009;42:312-3.
6. Ceriotti F. Laboratory quality regulations and accreditation standards in Italy. Clin Biochem 2009;42:317.
7. Shin BM, Chae SL, Min WK, Lee WG, Lim YA, Lee do H, et al. The Implementation and Effects of a Clinical Laboratory Accreditation Program in Korea from 1999 to 2006. Korean J Lab Med 2009;29:163-70.
8. Hui Li, Khosrow Adeli. Laboratory quality regulations and accreditation standards in Canada. Clin Biochem 2009;42: 249-55.
9. Bilic-Zulle L, Simundic AM, Supak Smolcic V, Nikolac N, Honovic L. Self reported routines and procedures for the extra-analytical phase of laboratory practice in Croatia – cross-sectional survey study. Biochem Med 2010;20:64-74.
10. Guzel O, Guner EI. ISI 15189 Accreditation: Requirements for quality and competence of medical laboratories, experience of a laboratory I. Clin Biochem 2009;42:274-8.
11. Yanikkaya-Demirel G. ISO 15189 accreditation: Requirements for quality and competence of medical laboratories, experience of a laboratory II. Clinical Biochemistry 2009;42:279-83.
12. Huisman W, Horvath AR, Burnett D, Blaton V, Czikkely R, Jansen RT, et al. Accreditation of medical laboratories in the European Union. Clin Chem Lab Med 2007;45:268-75.