Introduction
Cardiovascular disease (CVDs) is the number one killer world-wide, and about 50% of all deaths are associated with high blood pressure (1). Over the years, a series of high risk factors have been established for CVDs including hypertension, dyslipidemia, diabetes mellitus, age, unhealthy diet, physical inactivity, tobacco use and excessive use of alcohol (1). However, it is hard to fully understand the cardiovascular risk with only these risk factors (2,3). Newer biomarkers, including plasminogen activator inhibitor 1 (PAI-1) (4), brain type natriuretic peptide (BNP) (5), N-terminal prohormone of BNP (NT-proBNP) (6,7), C-reactive protein (CRP) (8), D-dimer (9,10), troponin I (11) and inflammatory mediators (12) have been associated with CVD risk. Patient stratification can be enhanced by measuring these biomarkers simultaneously (13).
Previously, we have quantified D-dimer concentrations in human saliva and demonstrated a two-fold increase in saliva compared with plasma collected from the same individuals (9). These findings prompted us to further investigate other proteins involved in the coagulation cascade. Thus, we investigated the PAI-1 concentrations in saliva. During coagulation, prothrombinase cleaves prothrombin into thrombin which transforms fibrinogen into highly self-adhesive fibrin monomers (14). The inhibition of fibrinolysis is performed by two types of PAIs: PAI-1 and PAI-2. A previous study has shown that there is tissue type plasminogen activator and PAI-1 activity in human parotid saliva (15). A more recent study using a commercial enzyme-linked immunosorbent assay (ELISA) kit detected the presence of only PAI-2, yet both PAI-1 and PAI-2 are expressed in salivary gland tissues (16).
Fibrinolytic deficiency is linked to a higher risk of developing CVDs including myocardial infarction (17) and coronary artery disease (18). Previous studies have demonstrated that high plasma PAI-1 concentrations are linked to myocardial infarction (17), stroke (19) and coronary artery disease (20). Thus, PAI-1 is considered as a useful biomarker for predicting the risk of coronary events (13).
Salivary secretions contain most of the biomolecules that are present in blood or urine (21-23). Saliva samples can be easily collected without the need for medical staff or hypodermic needles and saliva does not clot compared with blood, making the former biological fluid ideal for large population based screening studies. Additionally, saliva sample collection is very robust and saliva sample collection has significantly lower physiological and psychological impact on the donor than blood collections (8,24,25). Furthermore saliva can be collected and stored in stabilising solution several days later prior to being received by a testing centre. Saliva has even been used as a biological fluid for the diagnosis of ischemic heart disease (8), heart failure (6), in oral cancers (23). However, the concentration of the analytes in saliva are often much lower than in blood, and warrants higher sensitivity detection technologies. We hypothesise that human saliva contains PAI-1 and that the concentrations are not affected by the time of saliva collection (i.e. morning saliva sample vs. afternoon saliva). The aims were to adopt and validate an immunoassay to quantify PAI-1 concentrations in saliva and to determine whether saliva collection time has an influence in the measurement.
Materials and methods
Subjects
The University of Queensland Medical Ethical Institutional Board approved the protocol of this study and subjects provided written informed consent. We recruited 40 healthy subjects (20 males (19-36 years) and 20 females (19-25 years)) from the University of Queensland students and staff between August 22, 2012 and December 6, 2012. The subjects were of Asian and European descent, had good oral hygiene and showed no evidences of fever and/or respiratory tract infection. All subjects underwent a sample questionnaire which provided us with their medical history. In this study, we excluded subjects who have had any comorbid oral disease (e.g. periodontal disease and gingivitis), active infection, autoimmune disease, malignancy or who are smokers, undergoing dental treatment or any kind of medical treatment, denture wearers, pregnant and or had a recent operation or trauma. Written informed consents were obtained from all subjects before sample collection and none of the subjects were on any type of medication.
Samples
Saliva and blood samples from each subject were collected on the same day. Blood samples were collected into 4 mL sodium citrate tubes (Greiner VACUETTE® # 454327, Greiner Bio-one, Graz, Austria) by an experienced phlebotomist (Queensland Medical Laboratory Pathology Services, University of Queensland Blood Collection Centre). The blood samples were collected between 09.00 and 16.00 hours immediately after either the morning or afternoon saliva collection. Due to the impracticality of collecting multiple blood samples from the same subject, only one blood sample was collected from each subject. In order to obtain plasma, the blood samples were centrifuged at 1500 x g at room temperature for 15 minutes immediately after collection. The plasma samples were then aliquoted, de-identified and stored at -80 °C until analysis. Saliva samples were collected into sterile Falcon Polypropylene Conical Tubes (50 mL, BD Bioscience, #352070, San Jose, CA, USA). The saliva was collected by an unstimulated resting drool method which is well described in literature (26,27). In order to obtain a relatively constant baseline, we asked all subjects to stop eating and drinking (with the exception of water), one to two hours prior to saliva donation. We collected one saliva sample from each subject in the morning (08.00-12.00 hours) and one saliva sample in the afternoon (14.00-16.00 hours) to investigate the diurnal variation of PAI-1 concentrations. Similar to the saliva samples, all the plasma samples were aliquoted and de-identified immediately post collection. The saliva was then diluted 90% with 1X AlphaLISA(R) immunoassay buffer (Product-No: AL286 C/F, Perkin Elmer®, MA, USA) and stored at -80 °C until analysis.
The adoptation and the validation of PAI-1 AlphaLISA® Immunoassay
In this study we utilised a highly sensitive AlphaLISA® technology (PerkinElmer®, Boston, MA, USA). It is a homogeneous, bead-based sandwiched immunoassay that offers many advantages over traditional ELISA including relatively higher sensitivity, low sample volumes can be accurately analysed in a less labour consuming manner. The PAI-1 AlphaLISA® kit is validated for the use with human serum/ plasma samples and cell culture supernatants. This kit has not been validated to measure PAI-1 in saliva samples. In the first instance we performed a pilot study to determine likely PAI-1 concentration range. This was done to make sure that the background PAI-1 concentrations are low and that one is able to obtain a relatively higher signal to noise ratio. Saliva samples collected form healthy subjects were diluted using immunoassay buffer. Once the saliva concentration range was established, standards were prepared by diluting PAI-1 standard from the PAI-1 AlphaLISA® kit (Product-No: AL286 C/F, Perkin Elmer®, MA, USA) in a 90% saliva matrix, by using pooled saliva (9 mL) and 1 mL of immunoassay buffer from the kit. The matrix was prepared by pooling saliva from 10 healthy subjects. A standard curve was generated using twelve standards at the concentration of 1,000,000, 300,000, 100,000, 30,000, 10,000, 3,000, 1,000, 300, 100, 30, 10 and 3 pg/mL. Quality controls were also prepared in a similar manner by diluting a known concentration of PAI-1 in 90% saliva. The quality controls were analysed in the assay runs to provide recoveries. For the plasma measurement, the same strategy was used except that the standards were prepared in pooled plasma (N = 3, 0.1% of pooled plasma).
To measure the concentration of PAI-1 in plasma and saliva samples, in house adopted PAI-1 AlphaLISA® kit (Product-No: AL286 C/F, Perkin Elmer®, MA, USA) was used. It contains a biotinylated anti-PAI-1 polyclonal antibody, which binds to the streptavidin-coated donor beads while the anti-PAI-1 polyclonal antibody is conjugated to the acceptor beads. In the presence of PAI-1, the beads come into close proximity. After excitation at 680 nm, donor beads will give out singlet oxygen molecules that trigger a cascade of energy transfer in the acceptor beads, resulting in a sharp peak of light emission at 615 nm.
The samples were analyzed (triplicate) in 384 well ProxiPlatesTM (Perkin Elmer®, MA, USA). We decreased the total reaction volumes from 50 µL to 10 µL and changed the final concentration of streptavidin donor beads from 40 µg/mL to 12.5 µg/mL. Briefly, the immunoassay consisted of adding 1 µL of sample/analyte into a 384-well microplate, and then adding 2 µL of biotinylated antibody (10 nM) followed by a 30 minutes incubation at room temperature. After the first incubation, 2 µL of acceptor bead (100 µg/mL) was added, followed by 60 minutes incubation at room temperature. Since the streptavidin donor beads are light sensitive, 5 µL streptavidin donor beads (50 µg/mL) was added to each well under subdued laboratory lighting. The microplate was read using an EnSpire™ plate reader (Perkin Elmer®, MA, USA) after 30 minutes of incubation in the dark at room temperature.
Assay performance characteristics for the in house developed salivary PAI-1 AlphaLISA(R)
Recovery
Three known concentrations of commercial recombinant PAI-1 (Product-No: 1728540, Perkin Elmer®, MA, USA) were spiked in pooled saliva collected from healthy subjects (N = 4) in order to determine analyte recovery. Both spiked and un-spiked pooled saliva were measured in the same AlphaLISA(R)immunoassay. The percentage recovery of the three spiked saliva samples was calculated in reference to respective un-spiked pooled saliva samples in a single AlphaLISA(R)immunoassay, using the following equation (28):
Percentage recovery (%) = (PAI-1 concentration in spiked saliva — PAI-1 concentration in un-spiked saliva) / (amount of spiked PAI-1) × 100%
Intra-and inter-assay coefficient of variation for the PAI-1 AlphaLISA(R) assay
To determine intra- and inter- assay variations, triplicates of saliva samples from 40 healthy subjects were analysed in one AlphaLISA(R)PAI-1immunoassay run and then three independent AlphaLISA(R)PAI-1immunoassays runs, respectively (28). Intra- and inter-assay variations were expressed by intra- or inter- assay coefficient of variation (%CV). %CV was calculated using the following equation:
%CV= (Mean of SD) / (Mean) × 100%
Limit of detection and limit of quantification for PAI-1 AlphaLISA (R) immunoassay
To determine the assay’s limit of detection (LOD) and limit of quantification (LOQ), 9 blanks (2.5% pooled saliva diluted in 1X AlphaLISA Immunoassay buffer) were measured in one immunoassay run. The LOD and LOQ for the salivary PAI-1 immunoassay was read from a sigmoidal-dose response curve based on LOD and LOQ signal counts derived from the equations (29):
LOD signal count = (Average of black signalcount) + 3 × (standard deviation of blank signal)
LOQ signal count = (Average of black signalcount) + 10 × (standard deviation of blank signal)
Statistical analysis
All statistical analyses were performed using GraphPad Prism 5 software version 6.02 (GraphPad Software Inc., La Jolla, CA, USA). We generated a standard curve by plotting the “raw” AlphaLISA counts vs. the concentration PAI-1 analyte. The data was analyzed according to a nonlinear regression using a 4-parameter logistic equation (sigmoidal dose-response curve with variable slope) and a 1/Y2 data weighting.
For clinical characteristics (continuous variables) of the subjects, a Kolmogorov-Smirnov statistic was performed in order to test for normal distribution before statistical analyses. Mann-Whitney U tests and Wilcoxon tests were performed on unpaired and paired data without normal distribution to compare values from two groups, and Chi-square tests were performed for dichotomous variables. To investigate the relationship between salivary and plasma PAI-1 concentrations and in the morning and the in the afternoon samples, nonparametric Spearman product moment correlation coefficients were calculated. A P-value < 0.05 is considered to be statistically significant.
Results
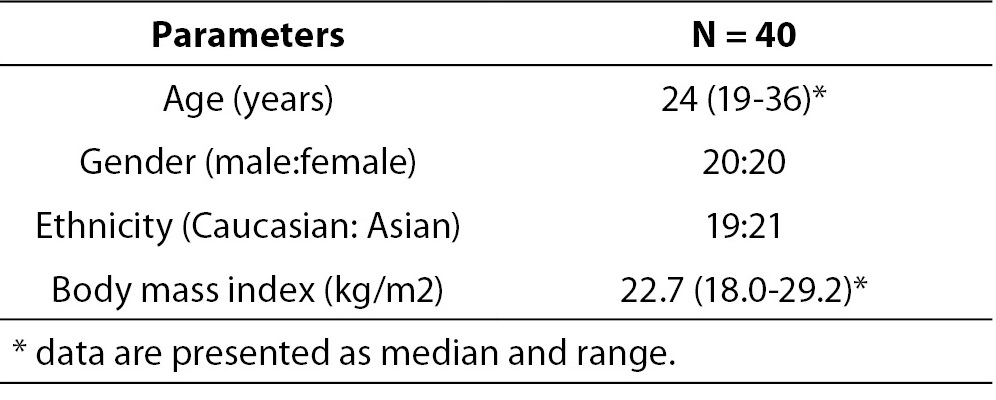
In total 40 healthy subjects were enrolled in the study. The details of the subjects are shown in Table 1. There were equal number of healthy men and women with median age 24 years and median body mass index 22.7 kg/m2.
Table 1. The biological characteristics of healthy control subjects recruited in this study.
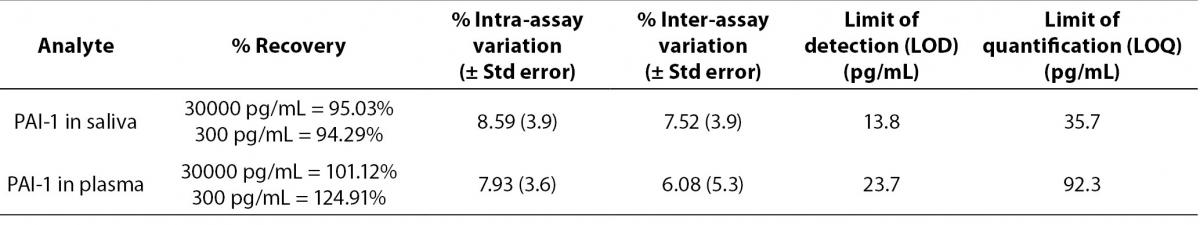
The performance characteristics of the PAI-1 immunoassay are summarized in Table 2. Also, the PAI-1 assay performed well with an acceptable analyte recovery expectations (75-125%) (30). In addition, both inter and intra-assay CVs were less than 10% highlighting the reproducibility of the assay.
Table 2. Performance characteristics of the adopted salivary PAI-1 AlphaLISA® immunoassay.
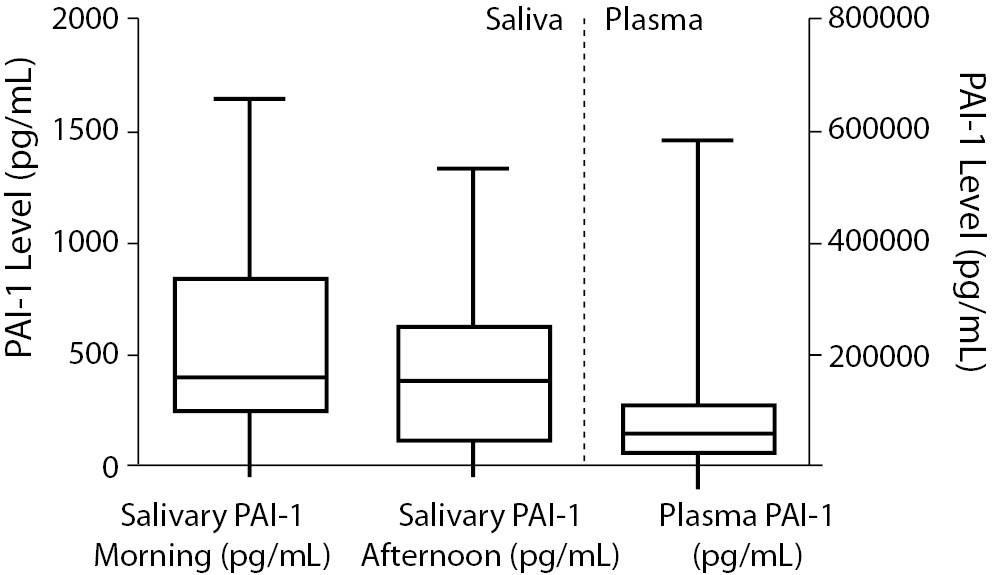
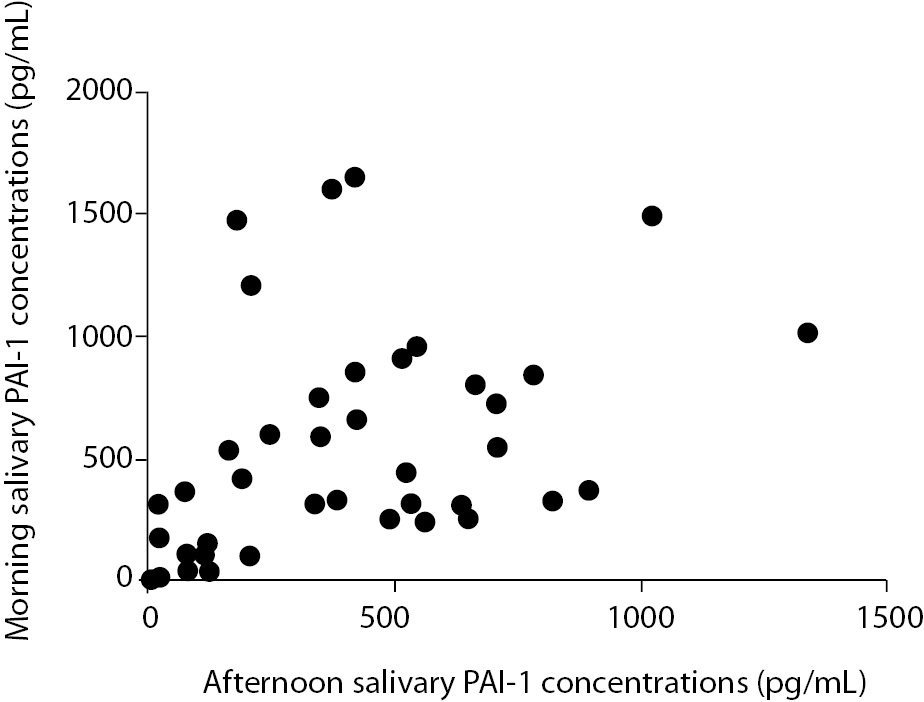
The PAI-1 concentrations in the saliva samples collected in the morning ranged between 13.8-1645.0 pg/mL with a median value of 394.4 (243.4-833.1) pg/mL (Figure 1). The PAI-1 concentration in the saliva samples collected in the afternoon ranged between 13.8-1331.0 pg/mL with a median value of 375.8 (129.1-615.4) pg/mL. There was no significant difference between PAI-1 concentrations in the saliva samples collected in the morning and in the afternoon (P = 0.108) (Figure 2). In fact, there was a significant correlation between the morning and afternoon samples (P = 0.001, Spearman r = 0.51, Figure 3).
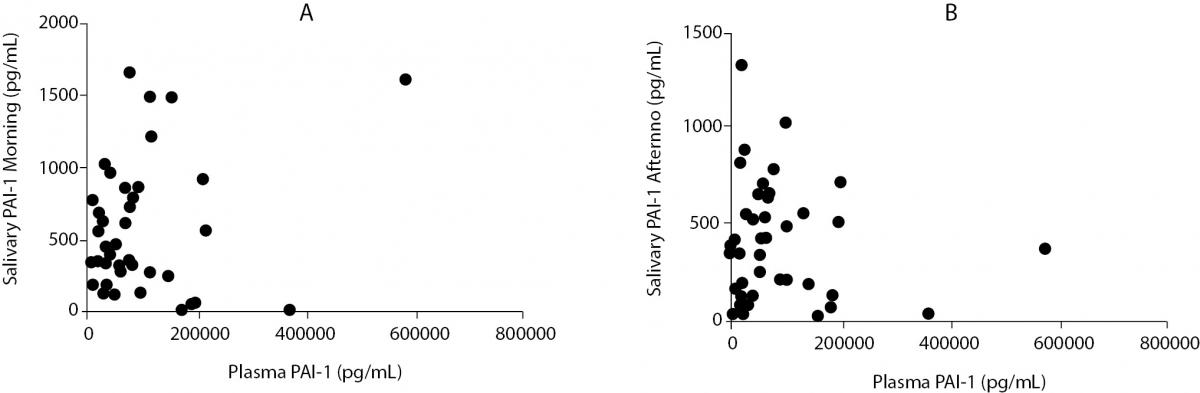
The PAI-1 concentration in the plasma samples ranged between 23.7-582,000 pg/mL with a median of 59000 (24,000-110,000) pg/mL (Figure 1). There was a significant difference between the morning and afternoon saliva PAI-1 concentrations and plasma PAI-1 concentrations, P < 0.001 (Figure 2). There was no correlation between plasma PAI-1 concentrations with either morning or afternoon salivary PAI-1 concentrations (P = 0.812 and P = 0.949, respectively) (Figure 3).
Figure 1. The concentrations of salivary PAI-1 and plasma PAI-1.
Figure 2. Comparison of PAI-1 concentrations in the saliva collected in the morning to the saliva samples collected in the afternoon (Spearman correlation coefficient r = 0.51, P=0.001).
Figure 3. The comparison of PAI-1 concentrations in plasma to (A) saliva samples collected in the morning (Spearman correlation coefficient r = 0.01, P= 0.949) and (B) saliva samples collected in the afternoon (Spearman correlation coefficient r = 0.04, P = 0.812).
Discussion
AlphaLISA® immunoassays have not been validated by the manufacturer to be suitable with complex biological matrices such as saliva. We have adopted the PAI-1 assay by performing calibration curves in saliva and calculating the analyte recovery by spiking saliva samples with PAI-1 analyte. The validation of the PAI-1 assay was carried out as per FDA guidelines (30). The PAI-1 assay performance characteristics were acceptable with regard to the assay dynamic range, analyte recovery and lower limit of detection. Salivary PAI-1 concentrations were not affected by the time of saliva collection. Salivary PAI-1 concentrations were significantly lower than plasma concentrations and there was no correlation between plasma and salivary PAI-1 concentrations.
PAI-1 is an important regulator of fibrinolysis at sites where vascular injury and thrombus formation occurs. In this study, we have demonstrated that PAI-1 concentrations are detected in saliva collected from non-smoking, young healthy subjects. Current assays to quantify PAI-1 concentrations in body fluids are validated to be used with plasma samples. The presence of PAI-1 in saliva has diagnostic potential and hence it is important to develop an immunoassay to reliably quantify this analyte. There was a significant correlation between morning and the afternoon PAI-1 salivary concentrations implying that the effect of circadian rhythm is minimal for PAI-1 in saliva. There was no correlation between salivary and plasma PAI-1 concentrations. One possible explanation could be that salivary PAI-1 has two sources of origin: in situ synthesized in the salivary acinar cells as well as the PAI-1 that get transported from the blood endothelium into salivary acinar cells. Diurnal variation of plasma PAI-1 concentrations has been reported previously (31) which strongly indicates salivary PAI-1 has a different origin rather than passive filtration from blood. A recent study demonstrated that tissue factor associated with exosomes in saliva has the ability to promote blood coagulation (32). Counterbalancing this is the presence of PAI-1 which can inhibit fibrinolysis. Further research is required to fully delineate the biological role of PAI-1 in unstimulated human whole saliva. The stability of PAI-1 in saliva at room temperature is not known. Our data demonstrated that at room temperature both recombinant PAI-1 and salivary PAI-1 remained stable for over 7 hours, and slightly degraded post 24-hours (9% loss after 24-hours, data not shown).
A study by Virtanen et al. (16) detected plasminogen activators and their inhibitors in cell free human saliva. They also showed the expression of PAI-1 and PAI-2 in normal human submandibular and parotid gland tissues (in both acinar and ductal cells) suggesting that these inhibitors are produced endogenously by salivary glands. However, in the study by Virtanen et al. they did not detect PAI-1 in human saliva (16). One reason for this discrepancy could arise from the sample of choice (in our study we used whole mouth unprocessed saliva and they used cell-free saliva supernatant). We have also demonstrated in the past that the method of saliva collection and processing has an influence on protein detection (24,25). A second reason could be that the method that Virtanen et al., used is less sensitive assay than the AlphaLISA® assay used in this study. A third reason could be due to the differences in the study subjects i.e. we investigated healthy non-smoking subjects as opposed to neurological out-patients.
In a previous study (9), we have demonstrated that D-dimer, a fibrin degradation product was present in unstimulated whole saliva collected from the same group of healthy subjects. When comparing the salivary PAI-1 concentrations and salivary D-dimer concentrations, we found a strong positive correlation between the two biomolecules (P < 0.001, r = 0.72). In theory, D-dimer concentrations and PAI-1 concentrations should be negatively correlated since D-dimer is a fibrin degradation product and PAI-1 is the inhibitor of fibrin degradation. Possible reasons for this positive correlation could be due to the fact that these two biomolecules have different origins and there is a lag time in the secretion of PAI-1 from salivary glands into actual saliva. Further studies are needed to shed light into the activities of these two biomolecules.
To improve our understanding of CVD, additional CVD risk factors such as newer biomarkers from distinct biological pathways are need to be investigated. Blood base markers have been widely used for the evaluation of CVD. However, blood is not necessarily an ideal diagnostic medium for population screening or first line test. The present study suggested that salivary PAI-1 assay has the potential to become an alternate screening test. Although this study using 40 healthy subjects has highlighted that salivary PAI-1 concentrations have potential, however further larger and long term study (including samples from CVD patients) need to be utilised to determine its clinical utility.
In summary, we have demonstrated that PAI-1 is quantifiable analyte in unstimulated saliva collected from healthy subjects which implied the potential clinical utility of a salivary PAI-1 test. The adopted PAI-1 assay produced acceptable precision, sensitivity and specificity. The concentration of salivary PAI-1 was significantly lower than plasma PAI-1 concentrations, and there was no correlation between salivary and plasma PAI-1 concentrations. These findings suggest that salivary PAI-1 may have different origins from plasma PAI-1.
This is a preliminary study to demonstrate that PAI-1 is detectable in human whole mouth saliva. One of the limitations of the present study is that we calculated the LOD of the immunoassay using data generated from 9 individual blanks instead of 20 as described in standard CLSI EP17-A2. Previous studies using this technology showed (data not shown) with 20 and 9 blanks showed very similar outcomes. Therefore, in order to reduce the amount of reagent used it was decided 9 blanks were sufficient to generate reliable data for calculating LOD. Another limitation of this study is that we did not include CVD patients. To establish a clinically reliable reference range guide of salivary PAI-1 concentration requires data from a large number of healthy controls. The next stage of the study should involve a much larger number of healthy controls and CVD patients to verify its clinical utility.
Acknowledgements
The authors would like to acknowledge the financial support from the University of Queensland Foundation Research Excellence Scheme, Queensland Centre for Head and Neck Cancer, University of Queensland Diamantina Institute internal strategic funds and the Queensland Government Smart Futures Fellowship Program (QGSFF). In addition, authors wish to acknowledge the clinical support from Queensland Medical Laboratory Pathology Services at the University of Queensland Health Centre.